Insomnia Treatment & Therapy with CBT-i
Stop fighting your sleep. Retrain it.
If you’re exhausted from “doing everything right” (sleep hygiene, supplements, earlier bedtimes, no screens) and you’re still wide awake at 2–4 a.m., the problem usually isn’t effort. It’s conditioning—your brain has learned that bed = alert, problem-solving, and pressure.
CBT-I (Cognitive Behavioral Therapy for Insomnia) is the first-line, evidence-based treatment for chronic insomnia. It works by changing the patterns that keep insomnia going—especially the behaviors and thoughts that accidentally train your nervous system to stay on high alert at night.
At STG Health, we provide CBT-I–informed insomnia psychotherapy that integrates nervous system settling with practical, data-driven sleep skills—so you can sleep with more consistency in real life, not just on “good nights.”
Sleep treatment is delivered by licensed clinicians and combines CBT-I protocols (including sleep scheduling and stimulus control), cognitive strategies, and mental health support into one coordinated approach. Our work focuses on helping you understand how your sleep system, thoughts, emotions, and physiology interact—and on building supports that are realistic, sustainable, and effective in daily life.
Not sure it’s insomnia? Start with Assessment
Quick Read (60 seconds)
CBT-I is first-line treatment for chronic insomnia (not just “sleep tips”).
The core levers are stimulus control + sleep consolidation (sleep restriction therapy), supported by cognitive work.
Sleep hygiene alone is not enough for chronic insomnia (it’s supportive, not curative).
Most standard CBT-I protocols are structured and time-limited (often 6–8 sessions), typically weekly/biweekly.
At SaskSleep, you’ll get 50-minute sessions, a sleep diary, and a practical plan you can implement immediately.
Does any of this feel familiar?
You might be a strong fit for individual CBT-I if you recognize patterns like:
- You’re tired… but the moment you lie down, your mind switches on
- You fall asleep, but wake up and can’t get back to sleep
- You dread bedtime because it feels like another performance test
- You spend more time in bed trying to “catch up,” and sleep gets worse
- You’re relying on medications/supplements and still feel stuck
- You’re functional on the outside, but privately running on fumes
Many adults with insomnia don’t just lose sleep—they lose trust in their own body. After years of forcing routines, chasing the “right” solution, and feeling like bedtime is a test they keep failing, insomnia often starts to amplify:
CBT-I therapy helps you shift from “What’s wrong with me?” to “What’s maintaining this pattern?”—and from surviving each night to rebuilding a sleep system that holds up under real life.
The missing piece most sleep advice ignores
Most sleep advice is hygiene-based: caffeine, screens, bedtime routine, the “perfect” environment.
Helpful—but incomplete.
Chronic insomnia is often maintained by two powerful forces:
Conditioned arousal: bed becomes a cue for wakefulness (not sleep)
Sleep pressure disruption: time in bed and irregular patterns weaken the body’s natural sleep drive
That’s why CBT-I works: it doesn’t just soothe you. It re-trains the system using the same learning principles that created insomnia in the first place—especially stimulus control and sleep consolidation.
Why we treat Insomnia this way
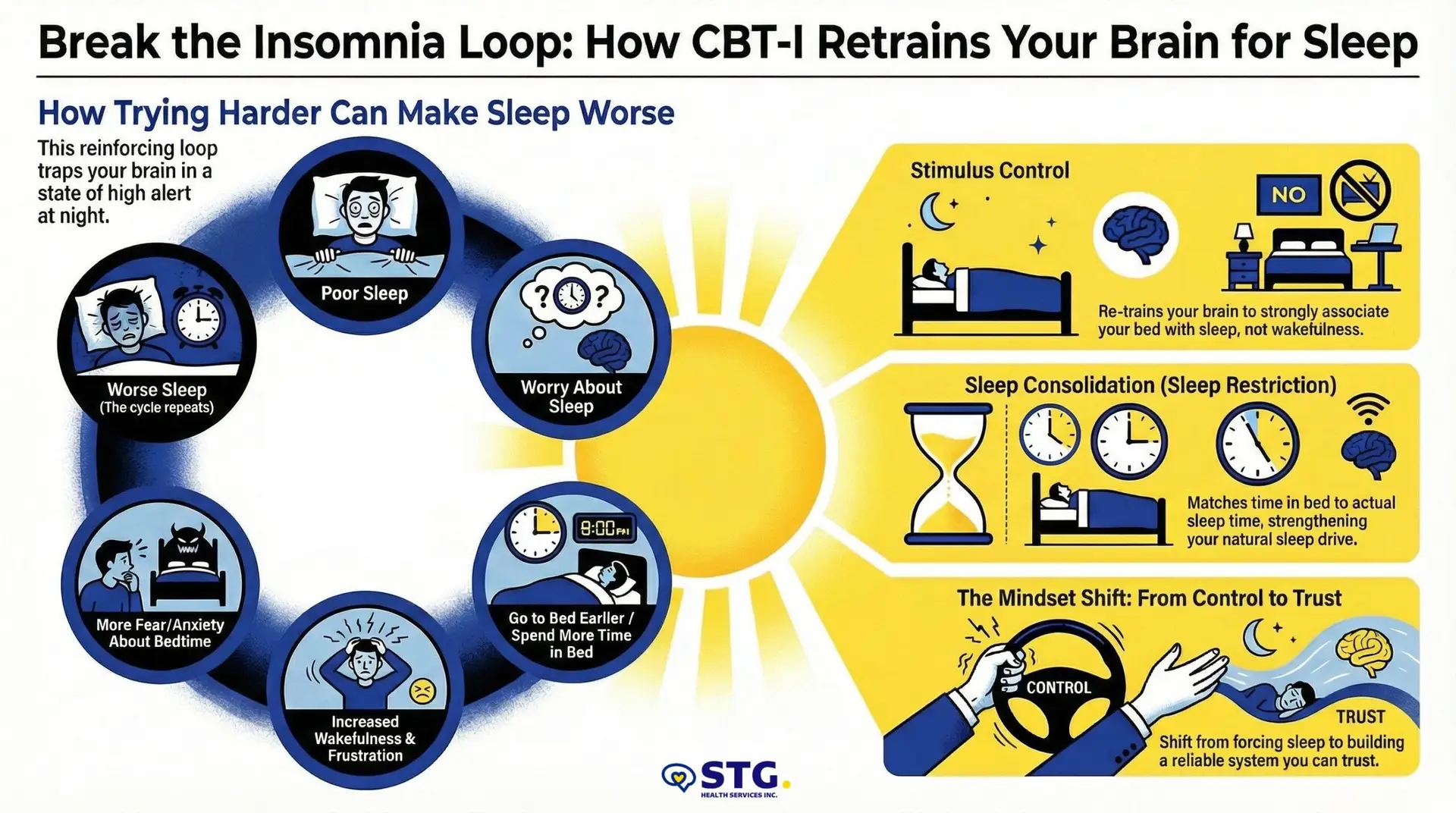
Many clients arrive having tried everything, yet they’re still trapped in the same loop:
Poor sleep → worry about sleep → earlier bedtime / more time in bed → more wakefulness → more fear → worse sleep.
The turning point is recognizing this isn’t a personal failure. Insomnia is often a learned pattern—and learned patterns can be unlearned.
CBT-I is recommended as initial treatment because it’s effective and tends to have fewer harms than long-term medication strategies.
The three shifts that make change sustainable
Shift 1 — From “Why can’t I sleep?” to “What’s keeping my system activated?”
We map what’s happening with precision: sleep timing, arousal patterns, conditioned cues, and the beliefs that fuel pressure at night.
Shift 2 — From “I need more time in bed” to “I need the right sleep window”
Counterintuitive but central: we adjust time-in-bed to rebuild sleep drive and consolidate sleep. This is a core CBT-I mechanism.
Shift 3 — From “I must control sleep” to “I can trust the process”
We shift from chasing perfect sleep to building reliability—so wake-ups don’t become spirals.
Which shift feels most true for you right now?
Treatment Options
Option A — Individual CBT-I Sleep Therapy
(recommended for complex insomnia)
Best for: chronic insomnia, sleep anxiety, middle-of-the-night awakenings, early waking, and insomnia that’s intertwined with stress, perfectionism, or overthinking.
This is structured, skills-based psychotherapy using CBT-I principles and a clear plan. CBT-I typically includes stimulus control + sleep restriction therapy (sleep consolidation) supported by cognitive strategies and targeted education.
If you feel like you’ve tried everything, your sleep has become fragile, and bedtime triggers pressure or fear—individual CBT-I is often the fastest way to personalize and stabilize progress.
Your plan is individualized, but commonly includes:
Sleep diary + pattern mapping (so we treat the real problem, not guesses)
Stimulus control (rebuilding bed = sleep)
Sleep consolidation / restriction therapy (strengthening sleep drive)
Cognitive restructuring (defusing catastrophic sleep thoughts)
Wind-down and arousal reduction (targeted, not generic)
Relapse-prevention plan (so setbacks don’t become resets)
This isn’t “talk therapy about sleep” and it’s not “try harder.” It’s collaborative, structured, and reality-based: small changes, tested weekly, adjusted with data.
At SaskSleep, individual CBT-I includes 50-minute sessions, a sleep diary, and between-session support.
Sleep hygiene is supportive—but on its own, it’s not an effective stand-alone treatment for chronic insomnia. CBT-I targets the mechanisms that maintain insomnia.
Not necessarily. We start with intake and screening to confirm fit and rule out other contributors that may need medical follow-up first.
Option B — CBT-I Group Program
(more affordable, structured support)
Prefer to learn alongside others and reduce cost? SaskSleep also offers a 6-session CBT-I group program.
What you Get
(a clear, tangible sleep plan)
When you begin individual CBT-I at SaskSleep, your plan may include:
Clinical sleep formulation — your maintaining loop, triggers, and sleep schedule
A personalized sleep window — adjusted week to week using sleep efficiency data
Stimulus control plan — exact rules for bed/awake time to recondition sleep cues
Cognitive plan — how to respond to nighttime thoughts without fueling arousal
Between-session practices — brief assignments that create momentum (not busywork)
Relapse prevention — what to do when sleep wobbles (travel, stress, illness)
What to Expect
(simple, predictable steps)
Step 1 — Book an intake
A short call to understand what’s happening, what’s been tried, and whether CBT-I is the best match.
Step 2 — Assessment + baseline sleep diary
You’ll complete brief screening and start a sleep diary so we can treat patterns precisely (not generically).
Step 3 — Build your CBT-I plan
We set your first sleep window and stimulus control plan, and decide what to target first (sleep onset, wake after sleep onset, early waking, sleep anxiety).
Step 4 — Weekly adjustments + stabilization
We refine week by week. It’s common to see meaningful change as the system relearns sleep—often with a short initial phase where fatigue can temporarily increase as the sleep window tightens.
Do I Need a Formal Insomnia Diagnosis?
If you already know you’re dealing with chronic insomnia, we can begin treatment right away.
If you’re not sure what’s driving your sleep difficulty, you still have options:
Start with an Intake & Sleep Assessment to clarify what’s going on and determine whether CBT-I is the best fit.
If you’re awaiting medical testing or specialist input, we can discuss interim supports to reduce sleep anxiety and stabilize your routine during that window.
STG Online Clinic
(included for clients)
As part of your insomnia care, you may also receive access to the SaskSleep CBT-I Online Course—a secure, self-paced program inside our STG online clinic. The course includes 32 short lessons designed to support your treatment by helping you understand the “why” behind CBT-I and giving you practical tools you can return to between sessions.
The online course is not a replacement for therapy or medical care. Think of it as your “between-session support system”: it reinforces the work we do together, helps you stay consistent when motivation dips, and gives you structure when sleep feels unpredictable.